If you’ve taken a neuroanatomy course, you know the feeling. Dense terminology, spatial relationships that don’t translate from flat diagrams, and a volume of material that can feel impossible to retain. Medical students consistently rank it among the hardest subjects in their education (Hall et al., 2018; Qamar et al., 2021), and the anxiety it creates has its own name: “neurophobia.” But it’s also one of the most rewarding subjects to learn well. Here’s why it matters and what makes it so hard.
What Neuroanatomy Covers
Neuroanatomy is the study of the nervous system’s structure. It spans scales, from individual neurons up to whole organs like the brain and spinal cord, covering the central nervous system (CNS) and peripheral nervous system (PNS), the pathways connecting them, and the clinical significance of each region. It also draws on histology, physiology, and molecular biology, which is part of why the learning curve is steep.
Why It Matters Clinically
Diagnosing neurological disorders often starts with a physical exam. Muscular weakness, numbness, or abnormal eye movements can point to a specific location in the nervous system. A provider who understands the anatomy can localize the problem, order the right imaging (CT, MRI, EEG, nerve conduction), and act quickly. In conditions like stroke, that speed saves lives.
This isn’t just a skill for neurologists. Physicians, PAs, NPs, nurses, therapists, dentists, psychologists; anyone in healthcare encounters patients with neurological symptoms. All medical students go through an intensive 2-3 month neuroanatomy curriculum, and it shows up on board exams like the USMLE and COMLEX. The need keeps growing: approximately 11 million people die from neurological disorders every year (WHO, 2025).
How Students Learn It
The traditional toolkit includes lectures, textbooks, anatomical atlases, and cadaveric dissection (though many schools have cut lab time due to cost). Students work at both macro and micro scales: surface anatomy of the cortex and brainstem, cross-sections revealing internal architecture, and imaging like MRI and CT that shows the living nervous system. Clinical correlation sessions tie it together by connecting classroom learning to real patient cases.
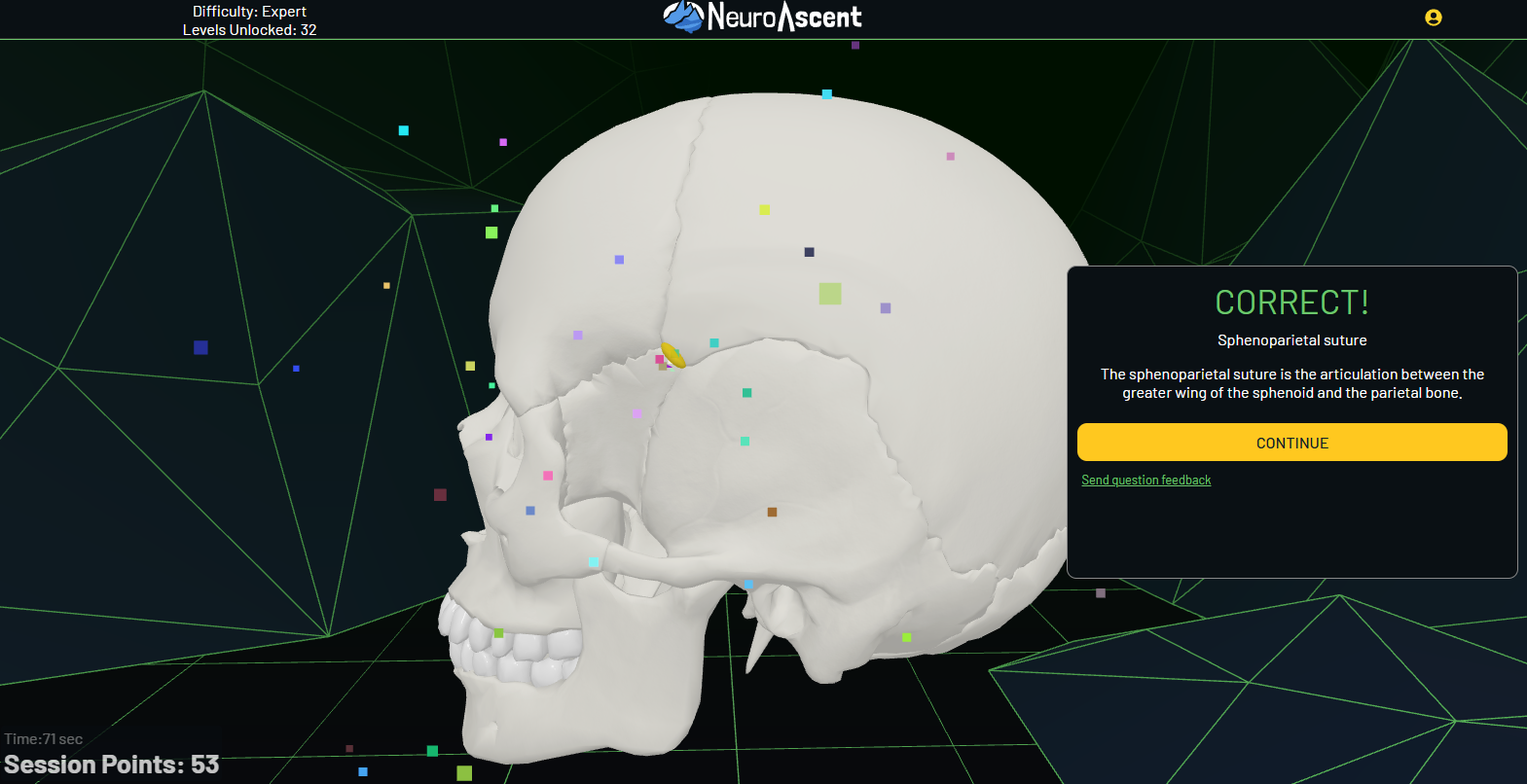
What’s been missing is good digital tooling. Most medical disciplines have interactive resources. Neuroanatomy has lagged behind, which is a problem for a subject where 3D spatial understanding is so important. That gap is exactly what we built NeuroAscent to address.
References
Hall S, Stephens J, Parton W, et al. Identifying Medical Student Perceptions on the Difficulty of Learning Different Topics of the Undergraduate Anatomy Curriculum. Med Sci Educ. 2018;28(3):469-472. doi:10.1007/s40670-018-0572-z.
Qamar K, Bashir S, Khalid R, Abaid M, Khadim R. Reasons for Difficult Topics in Anatomy and Their Solutions as Per Undergraduate Medical Students. Khyber Med Univ J. 2021;13(3):161-165. doi:10.35845/kmuj.2021.21177.
WHO. 11 million lives lost each year: urgent action needed on neurological care. Geneva: World Health Organization; 2025 Oct 14. Available from: https://www.who.int/news/item/14-10-2025-11-million-lives-lost-each-year-urgent-action-needed-on-neurological-care.